Customer expectations in insurance have changed faster than support systems. Policyholders now expect instant answers, real actions, and continuity across chat, voice, and email - whether they're filing a claim, updating coverage, or checking a payment.
Traditional chatbots were built to answer questions. Modern AI agents are built to complete work. This difference is redefining insurance customer experience.
While both chatbots and AI agents aim to improve service, only agentic AI can reason, connect to core systems, and execute multi-step insurance workflows. For insurers handling high-stakes interactions like claims, billing disputes, and endorsements, this capability is no longer optional.
Conversational AI in insurance spans a wide spectrum, from rule-based bots that follow scripts to agentic AI systems that understand intent and take action.
The objective is the same: fast, accurate help for policyholders. The approach on the other hand, is completely different.
A chatbot typically retrieves information, whereas an AI agent can interpret policy context, trigger workflows, and resolve cases end-to-end.
This shift is especially critical in insurance, where a conversation often involves compliance, identity verification, and backend actions, not just FAQs.
- "Am I covered for flood damage from last week?"
- "Can I add my spouse to the policy effective today?"
- "Why was my claim partially rejected?"
- No understanding of policy context
- Cannot remember earlier interactions
- Require manual script updates
- Unable to complete real transactions
- Frequent handoff to human agents
- Update personal details like address or nominee
- Modify coverage or add endorsements
- Initiate or progress a claim
- Process payments or refunds

Menu-Driven Workflows and Predefined Responses
This structure works for basic information retrieval but struggles the moment a customer steps outside the script, with questions like:
Limitations of traditional chatbots:

Shallow Integration with Core Insurance Systems
Insurance operations rely on multiple core platforms, such as policy administration, claims management, billing engines, and CRM records. When bots only sit on the surface, customers are left in a loop: they can ask questions, but they can't get things done.
As a result, policyholders still need human agents to:
- Understand intent from free-form language
- Verify customer identity securely
- Retrieve policy and claims data in real time
- Trigger backend workflows
- Learn from ongoing interactions
- Understand mixed or incomplete questions
- Remember earlier interactions in the same case
- Answer using actual policy details, not generic text
- Adjust tone when a customer sounds worried or frustrated
- Continue a conversation days later without starting from zero
- Policy and coverage details
- Claim progress
- Past conversations
- Payments and renewals
- Risk or sentiment signals
- Warn before a policy lapses
- Flag missing claim documents early
- Catch mismatches in FNOL details
- Suggest next steps like inspections or endorsements

What Makes AI Agents Different
For example:
A customer says, “I crashed my car yesterday, am I covered?”
An AI agent can verify the policy, check coverage limits, initiate FNOL, request photos, and create the claim - all in the same conversation, without waiting for a human handoff.
On platforms like Nugget, AI agents handle end-to-end tasks such as claim initiation, policy changes, and payment updates, resolving up to ~80% of routine inquiries independently, while escalating sensitive cases to human teams with full context.
| Dimension | Traditional Chatbots | AI Agents (e.g. Nugget) |
|---|---|---|
| Understanding | Keyword & menu-based | Contextual reasoning with LLMs |
| Action Capability | Shares links only | Executes claims, updates, payments |
| Memory | No session context | Remembers history (Customer 360) |
| Integrations | Read-only APIs | Bi-directional workflow execution |
| Channels | Basic chat/IVR | Multilingual voice + chat unified |
| Compliance & QA | Manual sampling | 100% AI-driven monitoring |
| Escalation | Blind transfer | Context-rich human handoff |

Natural Language + Context Memory
AI agents are built for that reality. They can:

Omnichannel Customer 360 with Nugget Lifeline
Nugget Lifeline connects all of this into one Customer 360 view, visible to both AI and human teams. This includes:

Proactive Service & Risk Detection
AI agents flip that model. They can:
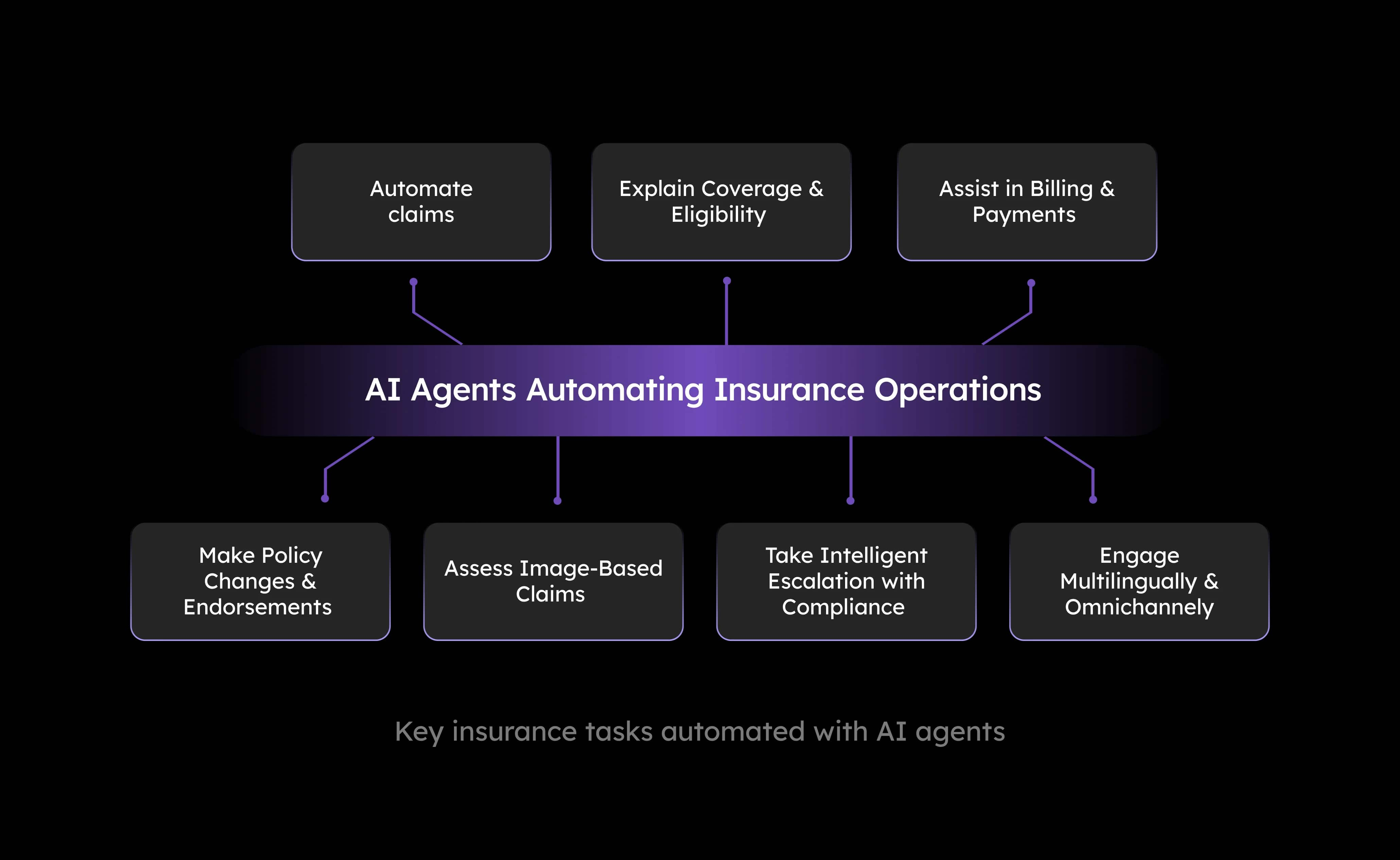
- Guide FNOL step-by-step
- Collect photos & documents
- Validate coverage
- Update claim systems
- Share real-time status
- Inclusions/exclusions
- Deductibles
- Sub-limits
- Renewal terms
- Due date reminders
- Payment retries
- Charge explanations
- Secure payment links
- Instalment changes
- Add drivers
- Change address
- Modify sum insured
- Update nominees
- Assess vehicle/home damage
- Classify severity
- Route to straight-through repair
- Flag fraud risks
- FNOL over phone
- Regional language support
- Natural, empathetic conversations
- Secure authentication
- Detect frustration/risk
- Escalate with full context
- Attach transcripts + actions
- Maintain audit trails

Claims Automation
Chatbot: "Here's the claims form."
AI Agent: "I've opened claim #4582, uploaded your photos, and scheduled inspection for tomorrow."

Coverage & Eligibility Explanations
AI agents can interpret:

Billing & Payments

Policy Changes & Endorsements

Image-Based Claims Assessment

Multilingual Voice AI

Intelligent Escalation with Compliance
Insurers adopting AI agents are seeing measurable improvements across operations:
- 40-60% faster resolution for routine cases
- Higher FCR with context-rich handoffs
- Lower cost per contact through automation
- 100% QA coverage via AI review
- Better CSAT through consistency
- Fraud & risk signals from conversation analytics
Insurers often hesitate to adopt AI because of concerns around legacy system integration, data privacy, and strict regulatory compliance.
Nugget addresses this with:
- API-first connectors
- Role-based governance
- Secure PII handling
- Audit-ready workflows
Adoption can be incremental; start with claims or billing, expand across journeys.
Chatbots answer, while AI agents resolve.
Insurance CX now demands systems that can reason, act, and orchestrate across claims, policies, billing, and voice. Nugget's agentic AI enables insurers to automate real workflows while keeping humans in control.
The winners will be insurers who treat AI not as a chatbot upgrade but as their core service engine.
They automate FNOL, document collection, coverage validation, and updates, cutting cycle times while reducing human error.
